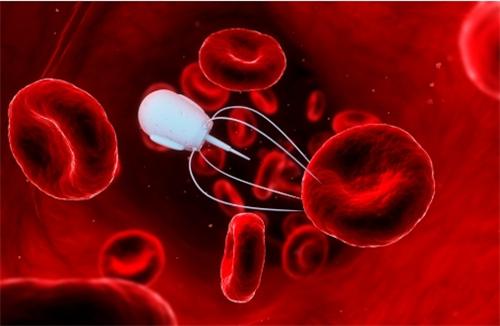
In November 2024, the Shenzhen Institute of Advanced Technology at the Chinese Academy of Sciences announced the successful completion of the world’s first human clinical trial of "nanorobots for cancer treatment." This groundbreaking technology uses micro-robots, each only 300 nanometers in diameter, injected into the patient's body via intravenous injection to precisely identify and eliminate circulating tumor cells in the blood. After three treatments with the nanobots, a terminal liver cancer patient showed a 98% reduction in tumor cell count in their blood, and tumor markers returned to normal levels.
Technology Behind the Nanorobots:
These tiny warriors are powered by three core technologies: magnetic iron oxide nanoparticles as the propulsion core, which are guided by an external magnetic field to move at a speed of 200 micrometers per second; nucleic acid aptamers on their surface as the "smart navigation system" to specifically identify biomarkers for 32 types of cancer; and on-board lytic proteins as "ammunition" that are released locally when encountering cancer cells. The most impressive feature is their collective intelligence — through near-field communication technology, tens of thousands of nanorobots can spontaneously form a "search-and-attack" network. The Max Planck Institute in Germany has praised this technology, stating, "This is the closest synthetic micro-nano system to living cells, achieving the perfect fusion of artificial and biological intelligence."
Advantages of Precision Treatment:
Compared to traditional therapies, the nanorobots show revolutionary advantages: the treatment is completely non-invasive, with patients only needing to lie in a magnetic navigation device for 90 minutes; side effects are minimal, with no significant adverse reactions observed during clinical trials; the precision is at the cellular level, allowing the distinction between cancer cells and normal cells, avoiding the indiscriminate damage caused by chemotherapy. Even more critically, they can bypass the blood-brain barrier, offering new solutions for brain cancer treatment. Dr. Li, an oncologist who participated in the trial, noted, "These nanorobots are like special forces, reaching metastatic sites that traditional drugs cannot, fundamentally blocking the pathways of cancer spread."
Clinical Application Prospects:
Currently, the technology has been approved for treating circulating tumor cells in the blood, a key factor in cancer metastasis. The next step is to develop an upgraded version that directly targets solid tumors by using micro-mechanical arms to physically destroy tumor tissue. The research team revealed that pancreatic cancer and ovarian cancer, two of the most aggressive cancers, will be the focus of future development. Biotech company NanoMed has already obtained the technology license and plans to release a commercial treatment system by 2026. Even more exciting is that this platform technology is highly adaptable and may be used in the future to clear blood vessel plaques, precisely deliver gene therapies, and more. Medical investor Chen Qiang predicts, "This will be the most significant breakthrough in cancer treatment since PD-1, with a market potential exceeding $100 billion."
Safety and Ethical Considerations:
Although the prospects are promising, the biological safety of the nanorobots still requires long-term monitoring. The main concern is that they could proliferate uncontrollably in the body or mistakenly attack normal cells. The research team has implemented three safety measures: biodegradable materials that ensure automatic decomposition after seven days; an internal "self-destruct switch" that responds to specific ultrasound signals; and strict limitations on the injection dose per kilogram of body weight. The Bioethics Committee is also concerned about the boundaries of "human enhancement" — whether this technology could be misused to create "nanoweapons" to modify healthy individuals. To address this, the World Health Organization is working on a "Global Governance Framework for Medical Nanorobots," and China has included it in the special regulation category of the "Biotechnology Safety Law."
Technical Challenges and Breakthrough Directions:
The current technology still faces three major bottlenecks: navigation accuracy drops by about 30% in deep tissues; the production cost is too high, with each treatment costing around $50,000; and the personalization adaptation cycle can take up to two weeks. The research team is developing an AI-assisted magnetic navigation system to improve precision, working on mass production to reduce costs, and building a cancer biomarker database to speed up adaptation. More advanced exploration involves giving the nanorobots "learning capabilities" so they can adapt to the evolution of cancer cells. The "fourth-generation" version, developed in collaboration with MIT, has shown potential against drug-resistant tumors in mouse experiments.
Future Medical Landscape:
Nanorobot technology is set to redefine the treatment paradigm. Scientists predict that by 2030, we may see "nanodoctors" that can stay inside the body long-term, continuously monitoring and eliminating abnormal cells; by 2040, "nanosurgical robots" may perform minimally invasive surgeries inside blood vessels; and in the more distant future, nanorobots may collaborate with immune cells to build a "cell firewall" in the human body.